Gum disease is one of the most common dental health problems in the United States — and one of the most under-recognized. Many people don’t realize their gums are in trouble until the condition has quietly progressed for months or even years. The good news? When you understand what’s happening at each stage, you have a real chance to stop it early, protect your teeth, and preserve your overall health.
This guide walks you through all four stages of gum disease — from the first signs of inflammation to the advanced bone loss that can lead to tooth loss — along with the symptoms to watch for and the treatment options available at every step.
What Is Gum Disease, and Why Does It Happen?
Gum disease, clinically known as periodontal disease, is a bacterial infection that affects the gum tissue and the structures that support your teeth. It starts when plaque — that sticky film of bacteria that forms on teeth every single day — isn’t fully removed through brushing and flossing. Over time, plaque hardens into tartar, which irritates and inflames the gums.
Left unaddressed, this inflammation gradually destroys the soft tissue and bone that hold teeth in place. What makes gum disease especially tricky is that it rarely causes serious pain in its early stages, so it’s easy to dismiss the early warning signs.
Certain factors can speed up the progression of gum disease, including:
- Inconsistent or improper brushing and flossing habits
- Smoking or using other tobacco products
- Uncontrolled diabetes or other systemic health conditions
- Hormonal changes (pregnancy, menopause)
- Certain medications that reduce saliva flow
- Genetic predisposition to periodontal problems
Understanding where you are in the disease’s progression is the first step toward getting the right care. At Pinnacle Dental’s comprehensive dental care practice, our team evaluates gum health at every check-up — because early detection makes all the difference.
Stage 1: Gingivitis — The Only Reversible Stage
What Is Gingivitis?
Gingivitis is the mildest and earliest form of gum disease. At this stage, the infection is limited entirely to the gum tissue — bone and other supporting structures haven’t been affected yet. That makes it the only stage of gum disease that is fully reversible with proper treatment and improved home care.
Symptoms to Watch For
- Gums that look red or puffy rather than a healthy pink
- Bleeding when you brush or floss (even light bleeding is not normal)
- Gums that feel tender or swollen to the touch
- Persistent bad breath that doesn’t go away after brushing
It’s worth noting that gingivitis doesn’t always hurt. Many people have it for years without noticing because the discomfort is minimal. That’s why routine cleanings and check-ups are so important — your dentist can spot the signs before you do.
Treatment at This Stage
A professional cleaning to remove built-up plaque and tartar, combined with a diligent at-home routine (brushing twice daily, flossing daily), is usually enough to reverse gingivitis completely. If you suspect your gums aren’t healthy, don’t wait — early intervention is easy and effective. You can also learn more about how scaling and root planing helps restore gum health when professional cleaning is needed.
Stage 2: Early Periodontitis — Infection Reaches the Bone
What Changes at This Stage?
When gingivitis isn’t treated, the bacterial infection spreads below the gumline. The body’s immune response begins attacking not just the bacteria — but the connective tissue and bone that hold teeth in place. Small “pockets” begin to form between the teeth and gums, typically measuring between 4–5 mm deep. This bone loss is not reversible, but it can be halted with the right treatment.
Symptoms at This Stage
- Gums that have started to pull away from the teeth (early recession)
- Increased sensitivity to hot or cold temperatures
- Gum pockets that your dentist can measure during a periodontal exam
- Ongoing bad breath despite good brushing habits
- Possible mild pain or discomfort when chewing
Treatment Options
The standard treatment at this stage is scaling and root planing — a deep-cleaning procedure that removes tartar and bacteria from below the gumline and smooths the root surfaces to help the gum tissue reattach. Antibiotic therapy may also be used to eliminate stubborn bacterial colonies. Regular follow-up visits become especially important here to monitor pocket depth and prevent further progression.
Stage 3: Moderate Periodontitis — Significant Bone and Tissue Loss
The Disease Deepens
At this stage, the infection has progressed significantly. Gum pockets typically measure 6–7 mm, and both bone and connective tissue loss are more substantial. The bacteria involved can also enter the bloodstream, which means gum disease at this stage is increasingly linked to systemic health concerns — including cardiovascular disease, diabetes complications, and respiratory issues.
Symptoms at This Stage
- Teeth may appear longer due to pronounced gum recession
- Noticeable looseness or slight shifting of teeth
- Deeper pockets that trap food and bacteria more easily
- Pus around the gum line in some cases
- Increased sensitivity and discomfort while eating
- Persistent, noticeable bad breath
Treatment Options
In addition to repeated deep cleanings, moderate periodontitis often requires more targeted intervention. Surgical options — such as flap surgery (to clean deep pockets) or bone and tissue grafts (to regenerate lost structure) — may be recommended depending on the degree of damage. Regular periodontal maintenance visits every 3–4 months become a long-term commitment at this stage.
💡 Did you know? Research has shown a strong connection between moderate-to-severe gum disease and a higher risk of heart disease, stroke, and poorly controlled blood sugar in people with diabetes. Protecting your gums isn’t just about your mouth — it’s about your whole body.
Stage 4: Advanced Periodontitis — Severe Damage and Tooth Loss Risk
What Makes Stage 4 Different?
Advanced periodontitis represents the most destructive phase of the disease. Pockets deepen to 8 mm or more, and the bone loss is severe enough that teeth may become too loose to save. This stage is not just a dental emergency — it’s a significant health concern that requires immediate, often surgical treatment.
Symptoms at This Stage
- Severe gum recession exposing significant portions of tooth roots
- Teeth that are visibly loose or have shifted position
- Pain when biting or chewing due to bone destruction
- Teeth that may fall out on their own or need extraction
- Jaw bone changes that can alter the shape of the face over time
- Persistent pus, swelling, and infection around multiple teeth
Treatment Options
At this stage, surgery is almost always necessary. Treatment may include full-mouth debridement, osseous surgery to reshape damaged bone, bone grafting, or guided tissue regeneration. In cases where teeth cannot be saved, tooth replacement options such as dental implants or dental bridges become part of the conversation. The goal shifts from reversing damage to preventing further loss and restoring function and appearance.
Patients who have experienced significant tooth loss due to advanced periodontal disease often explore restorative options. Understanding whether dentures or implants are better for long-term tooth replacement is an important step in rebuilding both function and confidence.
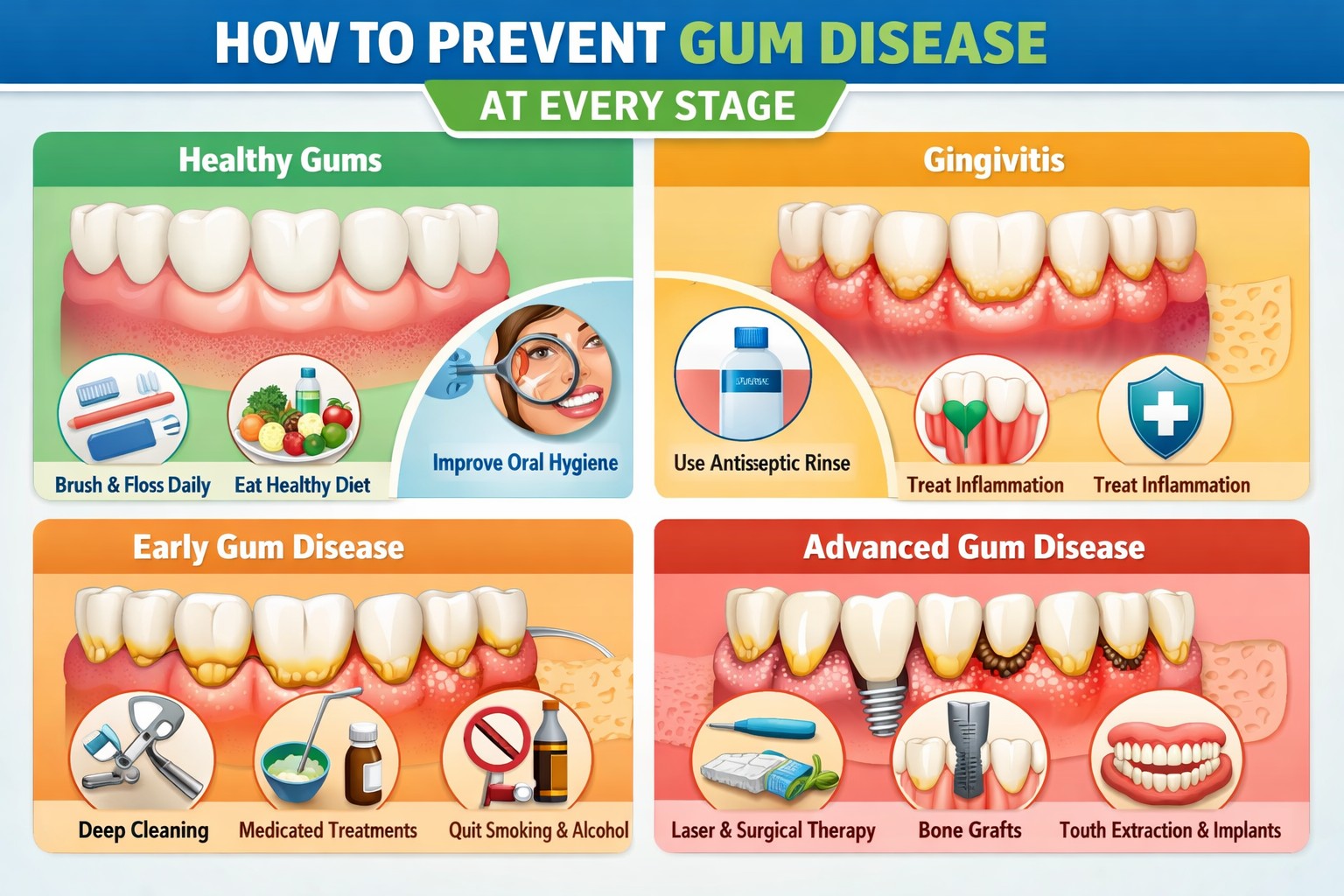
How to Prevent Gum Disease at Every Stage
Prevention is far simpler — and less costly — than treatment. Here are the most impactful habits for keeping your gums healthy:
- Brush properly twice a day using a soft-bristled toothbrush and fluoride toothpaste. Hold the brush at a 45-degree angle toward the gumline.
- Floss every single day — no shortcuts. Flossing removes plaque from areas your brush simply cannot reach.
- Schedule professional cleanings at least twice per year. Even the most disciplined brushers accumulate tartar that only a dental professional can remove.
- Quit smoking. Tobacco use is one of the biggest risk factors for gum disease and significantly slows the healing process.
- Manage chronic health conditions like diabetes, which can accelerate periodontal disease when poorly controlled.
- Stay hydrated and maintain good nutrition — a dry mouth creates a more hospitable environment for harmful bacteria.
If you’ve been putting off a dental visit, now is the right time to schedule one. Routine care through preventive family dentistry keeps minor gum issues from ever becoming major ones. For patients who experience dental anxiety, our team also offers comfortable sedation options to make every appointment stress-free.
Patients also sometimes notice early warning signs of oral infection through related symptoms. If you’ve been wondering whether persistent bad breath might signal a gum infection, that’s worth exploring — it persistent bad breath might signal a gum infection often is.
When Should You See a Dentist About Your Gums?
Don’t wait for pain. Pain is often a late symptom of gum disease, not an early one. Reach out to your dental provider if you notice any of the following:
- Gums that bleed during or after brushing or flossing
- Red, swollen, or tender gum tissue
- Persistent bad breath or a bad taste in your mouth
- Gums that appear to be pulling away from your teeth
- Tooth sensitivity that wasn’t there before
- Any tooth looseness or shifting
The earlier the problem is identified, the more treatment options are available to you — and the more likely you are to preserve your natural teeth. Our experienced team is here to provide a thorough periodontal evaluation and walk you through a personalized plan tailored to your oral health needs.
Concerned About Your Gum Health? We’re Here to Help.
Whether you’re noticing early signs of gum trouble or haven’t had a cleaning in a while, our dental team can give your gums a thorough evaluation and create a clear plan to get — and keep — your smile healthy.
Frequently Asked Questions
Can gum disease be cured completely?
Gingivitis — the first stage — can be fully reversed with professional cleaning and improved at-home care. However, once the disease advances to periodontitis and bone loss occurs, the damage is permanent. Treatment at later stages focuses on stopping further progression rather than restoring lost tissue. That’s why catching it early is so critical.
How do I know what stage of gum disease I have?
Only a dental professional can accurately stage gum disease. During a periodontal exam, your dentist or hygienist measures the depth of the pockets between your teeth and gums, checks for bleeding, evaluates bone levels using X-rays, and assesses recession and tooth mobility. These findings together determine the severity of the disease and what treatment is appropriate.
Does gum disease cause tooth loss?
Yes — advanced gum disease (Stage 3 and Stage 4) is one of the leading causes of tooth loss in adults. As the supporting bone and tissue are destroyed, teeth lose their anchor and can become loose, shift out of alignment, or need to be extracted. This is why treating gum disease early is so important for preserving your natural teeth long-term.
Is gum disease linked to other health problems?
Research has established strong associations between gum disease and several systemic health conditions, including cardiovascular disease, type 2 diabetes, respiratory infections, and complications during pregnancy. The bacteria involved in periodontal disease can enter the bloodstream and contribute to inflammation throughout the body. Treating gum disease is an important part of your overall health — not just your oral health.
How often should I get a dental cleaning if I have gum disease?
For patients with active or treated gum disease, most dentists recommend more frequent cleanings — typically every 3 to 4 months rather than the standard twice-yearly schedule. This is called periodontal maintenance, and it’s essential for preventing bacteria from rebuilding in the pockets between your teeth and gums. Your dentist will recommend a schedule based on the severity of your condition and how well you respond to treatment.
What is the difference between gingivitis and periodontitis?
Gingivitis is the earliest, mildest form of gum disease — it affects only the gum tissue and is fully reversible. Periodontitis is the term used for all stages that follow, where the infection has spread below the gumline and is actively destroying the bone and connective tissue that support your teeth. The key distinction is that gingivitis causes no permanent damage, while periodontitis does.
