Occasional bad breath is something most people experience after a strong meal or a restless night. But when that unpleasant odour lingers day after day — no matter how often you brush, it may be your mouth sending a more serious signal.
Gum infections, including early-stage gingivitis and the more advanced periodontal disease, often develop quietly. Bad breath can be among the first warning signs. Understanding the connection between oral bacteria, gum health, and breath quality can help you take action before small problems become larger ones.
What Causes Bad Breath?
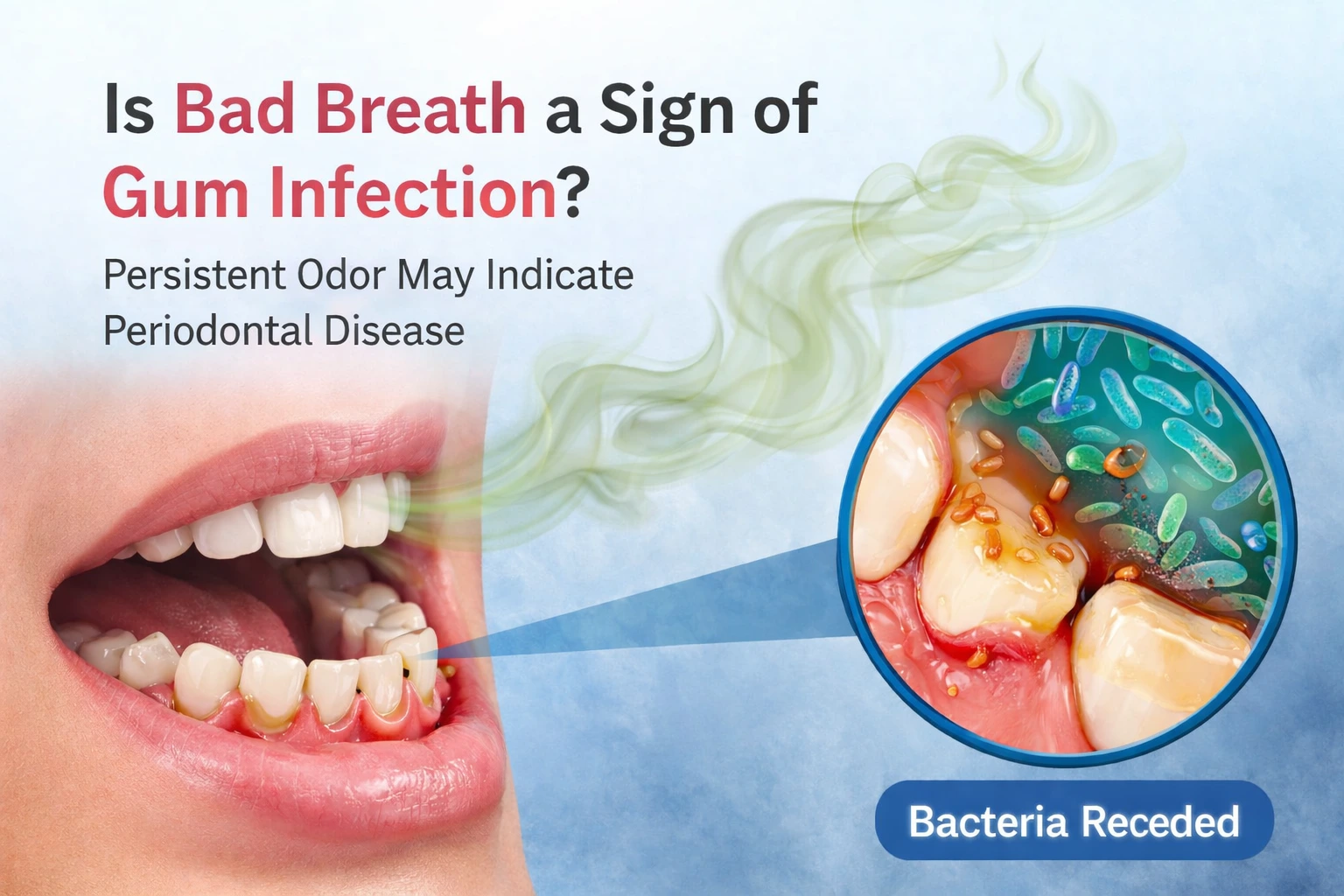
Most cases of bad breath start with bacteria in the mouth. The human mouth is home to hundreds of bacterial species, many of which feed on food particles left behind after eating. As these bacteria break down proteins and sugars, they release sulphur compounds — gases with a distinctly unpleasant smell.
Plaque and Tartar Buildup
When bacteria accumulate on teeth and along the gum line, they form a sticky film called plaque. Left undisturbed, plaque hardens into tartar, a rough mineral deposit that traps even more bacteria and is impossible to remove with brushing alone. This cycle of plaque and tartar buildup creates a persistent environment where odour-causing bacteria thrive.
Temporary Bad Breath vs. Chronic Halitosis
Temporary bad breath — the kind that follows a garlic-heavy meal or a morning coffee — is entirely normal and resolves quickly with good hygiene. Chronic halitosis, however, does not go away with brushing or mouthwash. It is a recurring, ongoing condition that often points to an underlying cause, such as a gum infection or untreated decay.
To understand the broader relationship between your mouth and your overall wellbeing, it is worth reading more about the importance of oral health: A guide to dental care.
What Are the Common Gum Infection Symptoms?
Gum disease rarely announces itself with obvious pain in its early stages. Instead, it reveals itself through a cluster of subtle but consistent signs. Recognising these early gum infection symptoms can make a significant difference in how quickly treatment is sought.
Bleeding or Swollen Gums
Healthy gums do not bleed. If you notice blood on your toothbrush or in the sink after flossing, this is one of the clearest early indicators of gum inflammation. Swollen, puffy, or red gums are equally important to watch for — they signal that bacteria have begun to irritate the gum tissue.
Persistent Bad Breath
As discussed above, bad breath that does not resolve with regular oral hygiene is a key symptom. In the context of gum disease, it is caused specifically by the toxins released by bacteria colonising beneath the gum line.
Gum Tenderness and Recession
Tenderness when eating or brushing, combined with the appearance that teeth are getting longer (a sign of gum recession), points to advancing gum disease. As infection progresses, the gums pull away from the teeth, exposing sensitive root surfaces and creating deeper pockets for bacteria to inhabit.
These symptoms, taken together, are the hallmarks of early to moderate periodontal disease. Catching them at this stage gives you the best chance of reversing or effectively managing the condition.
For a deeper look at keeping your gum tissue healthy, explore understanding the best practices for maintaining healthy gums. It is also wise to revisit how frequently professional evaluation is recommended —
When Do You Need Professional Treatment?
If you recognise any of the symptoms described in this article — particularly persistent bad breath combined with bleeding, swollen, or receding gums — it is time to see a dental professional. Gum disease treatment in Plano has advanced considerably, and today’s treatments are highly effective when the condition is caught before it becomes severe.
Deep Dental Cleaning
For patients with early to moderate gum disease, a deep dental cleaning is typically the first line of treatment. Unlike a standard cleaning that addresses the tooth surfaces above the gum line, a deep clean reaches into the periodontal pockets to remove accumulated plaque and tartar that standard brushing cannot touch.
Scaling and Root Planing
Scaling and root planing is the most common non-surgical treatment for periodontal disease. Scaling involves removing bacterial deposits from the root surfaces of the teeth, while root planing smooths those surfaces to discourage future bacterial attachment. This two-step procedure significantly reduces pocket depth, controls infection, and — critically for patients dealing with chronic halitosis — addresses the bacterial source of the odour directly.
Ongoing Preventive Dental Care
After active treatment, ongoing preventive dental care is essential to maintaining results. This typically includes more frequent professional cleanings (often every three to four months), periodic reassessment of pocket depths, and personalised home care recommendations.
An experienced dentist in Plano TX patients rely on will not only treat active gum disease but will also put a long-term management plan in place to ensure the condition does not progress further. Early and consistent professional care makes a measurable difference in outcomes.
How to Prevent Gum Infection and Bad Breath
Prevention is always preferable to treatment. The good news is that most gum infections — and the chronic bad breath they produce — are largely preventable with consistent habits and regular professional support.
Proper Brushing and Flossing
Brush for a full two minutes twice daily using a soft-bristled toothbrush, paying particular attention to the gum line where plaque tends to accumulate. Flossing once a day is non-negotiable — it removes food and bacteria from between the teeth where your brush cannot reach.
Healthy Diet Choices
What you eat affects both your breath and your gum health. Diets high in sugar feed the bacteria responsible for plaque and gum disease. Foods rich in vitamins C and D, calcium, and fibre, on the other hand, support healthy gums and saliva production — nature’s own oral rinse.
Don’t Let Chronic Bad Breath Go Unchecked. Contact Pinnacle Dental
Persistent bad breath is more than a social inconvenience — it is often a symptom that something deeper is happening in your mouth. Whether you are noticing bleeding gums, tenderness, or an odour that simply will not go away, these are signs worth taking seriously. Periodontal disease is a progressive condition, which means the earlier it is addressed, the better the outcome.
Choosing Pinnacle Dental for this kind of early evaluation means protecting not just your breath, but the long-term health of your teeth and the bone that supports them.
FAQs About Bad Breath Gum Infection
Is bad breath always a sign of gum disease?
Not always. Bad breath can result from a variety of causes including dry mouth, dietary choices, certain medications, sinus conditions, and even digestive issues. However, when bad breath is persistent and does not improve with brushing, flossing, or mouthwash, gum disease becomes a strong possibility and should be ruled out by a dental professional.
How do I know if I have periodontal disease?
The most reliable way to know is through a professional dental examination that includes measuring the depth of the spaces between your teeth and gums. However, common warning signs to watch for at home include gums that bleed easily, persistent bad breath, gum tenderness or swelling, teeth that appear longer than before (gum recession), and loose teeth in more advanced cases.
Can deep dental cleaning cure bad breath?
If gum disease is the cause of your chronic halitosis, then yes — deep dental cleaning, particularly scaling and root planing, can substantially reduce or eliminate the odour. By removing the bacterial deposits beneath the gum line that are producing volatile sulphur compounds, the source of the smell is directly addressed.
How often should I see a dentist in Plano for preventive dental care?
For most patients with healthy gums, professional cleanings and checkups every six months are the standard recommendation. However, patients who have been treated for periodontal disease or who are considered at higher risk are typically advised to attend more frequently — often every three to four months. Your dentist will assess your specific situation and recommend a schedule tailored to your oral health needs.
